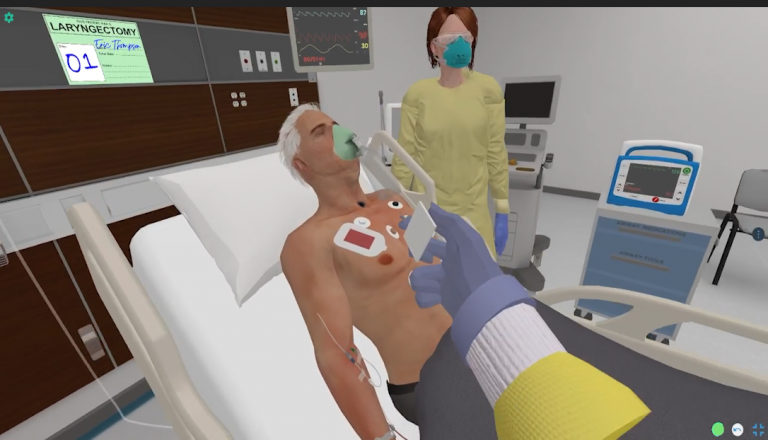
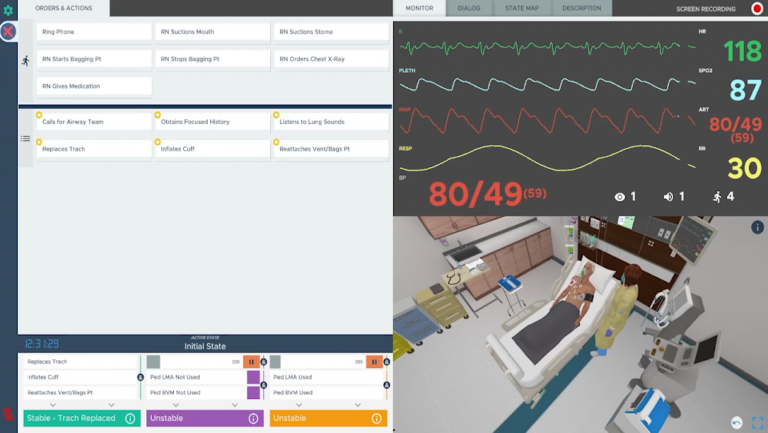
Similar Cases
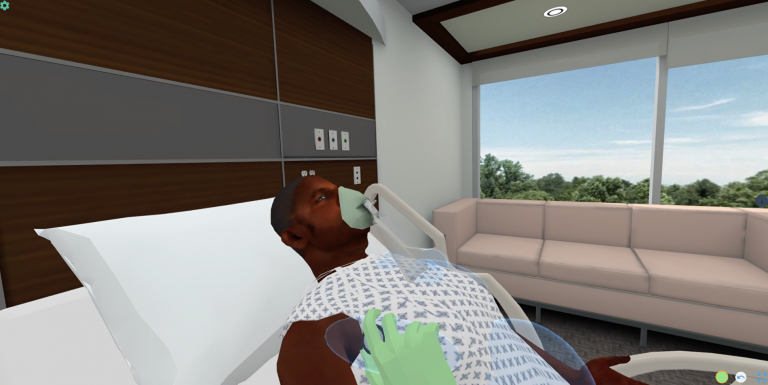
Geriatric Pneumonia—Inpatient
A 68-year-old male with COPD is admitted to the hospital with pneumonia; the...
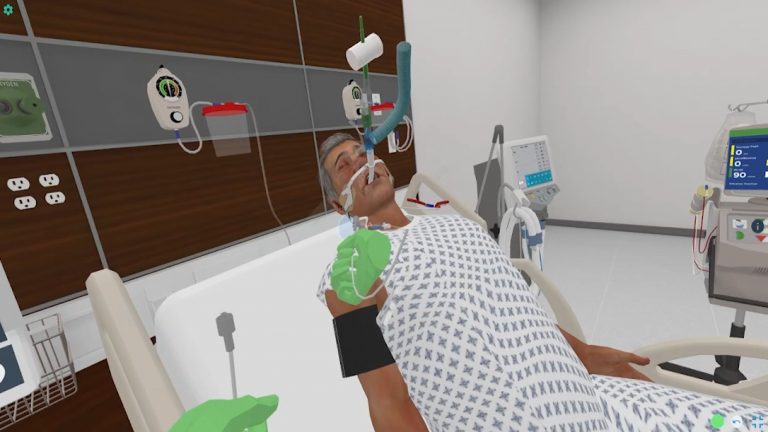
ICU Sepsis – CVVHD
Nick O. Kidman, a 54-year-old male patient admitted from ED for COPD exacerbation...

PALS Assessment And Resuscitation
A six-year-old boy presents to a community ED BIBA with mom in acute...
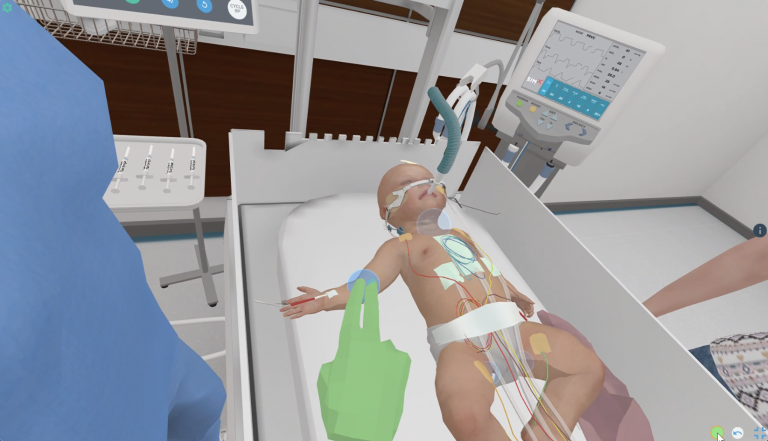
Pediatric Low Cardiac Output Syndrome
A 3 month-old infant s/p complete AV canal defect repair is recovering in...
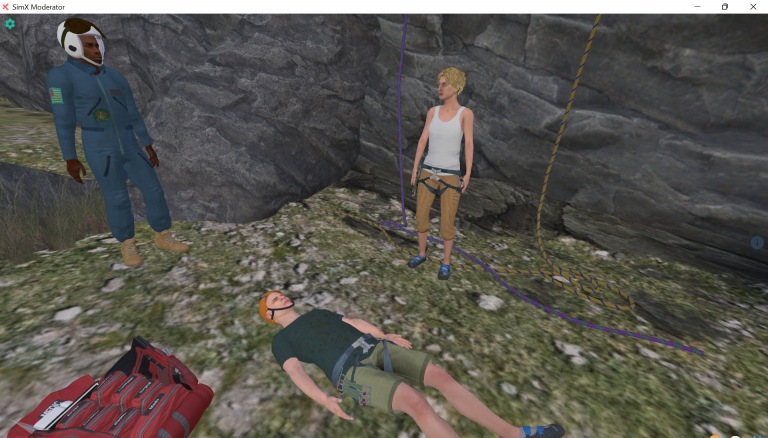
EMS Climbing Accident and Rescue
In this scenario, a 34 year-old male is involved in a climbing accident...

Infant with Bronchiolitis
A 4-month-old is admitted with RSV and bronchiolitis by their mother who is...

EMS Anaphylaxis with Difficult Airway
Learner will arrive on-scene to find a 53-year-old female patient lying on the...
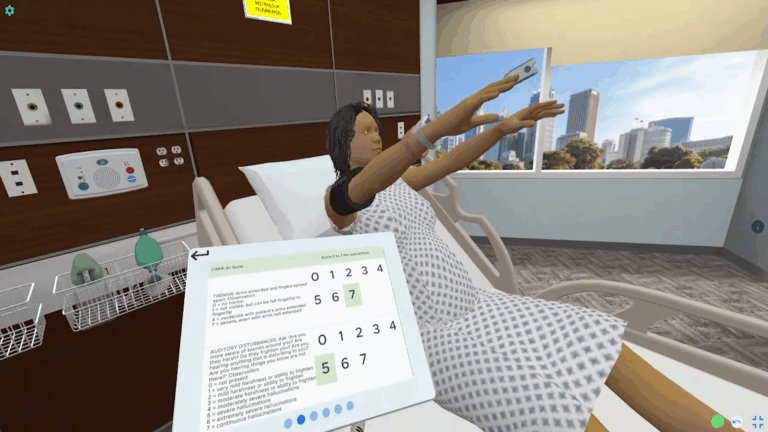
Alcohol Withdrawal, CIWA
Molly Maple is a 52 year old who came through the ER. She...

Intubation of Pediatric Patient with Suspected COVID
In this scenario, a patient with a history of repaired congenital heart disease...
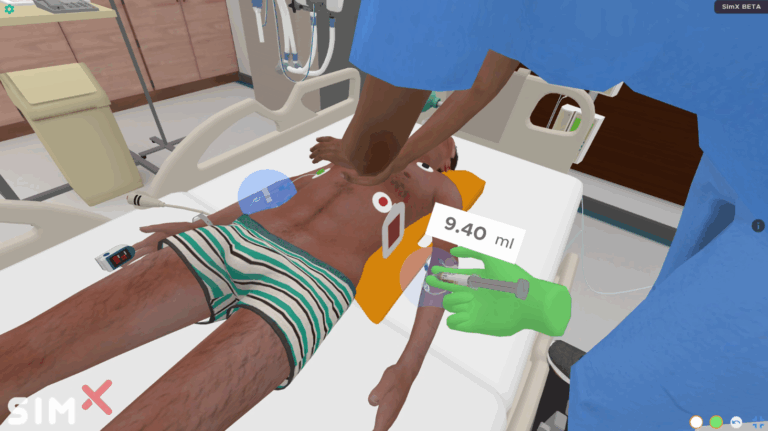
Sudden Onset Respiratory Distress
A 16-year-old with Duchenne Muscular Dystrophy with tachycardia, tachypnea and hypoxemia, found to...